Abstract
Background: Mind–body practices have a variety of health implications, including inflammatory modulation, cognitive improvement, and impact on neurofunction. Some of these effects have been demonstrated through rapidly developing technology and their impact on circulating blood levels of hormones and other molecules. As neurotrophic factors like brain-derived neurotrophic factor (BDNF) and hormones such as cortisol have been shown to play a role in cognitive function, this pilot study assessed the influence of a mind–body intervention, Qigong, on circulating levels in participants.
Methods: Participants were prospectively enrolled to perform three separate cognitive assessments before and after a 30-minute, self-guided Qigong meditation developed from historical literature. Each participant was assigned to one of two groups according to their level of experience with meditation. Circulating levels of BDNF and cortisol were analyzed before and after the intervention. Group-level mean changes in BDNF and cortisol, as well as mean change in cognitive assessment score, were compared between groups using t-tests.
Results: Fourteen participants were enrolled with equal allocation to the two groups. Though BDNF increased in inexperienced meditators and decreased in experienced meditators after Qigong, there were no differences in the mean change between groups. Similarly, no differences were noted in cortisol between groups; however, there was a significant reduction in all participants after Qigong (n=14, P=0.001). No significant difference in cognitive assessment was noted between groups after Qigong compared to baseline.
Conclusion: This pilot study provides preliminary data to suggest circulating levels of cortisol may respond to Qigong meditation. While we were able to indirectly measure cognitive function and directly measure circulating levels of BDNF, the small sample size in this study did not allow us to determine the relationship with Qigong. Larger studies are needed to expand on these findings.
INTRODUCTION
Mind–body exercises such as meditation and mindfulness have long been believed to promote health and recent technologies have enabled the elucidation of such benefits through objective measures. Growing research has shown that these mind–body interventions have effects on cognitive performance, physical markers of inflammation, and brain health. 1 , 2 Qigong is a system of mind–body practice that integrates physical postures, breathing techniques, and focused intentions to circulate life energy (qi or ch’i), with the purpose of restoring balance and health within the physical and psycho-emotional bodies. 3 As a meditative practice, Qigong distinguishes itself from stationary meditative practices by regular incorporation of gentle movement and, in some styles, sound and self-massage. 4
One marker of brain health is brain-derived neurotrophic factor (BDNF), classified as a “neurotrophin” due to its ability to modulate the nervous system’s excitatory and inhibitory neural pathways. BDNF also stimulates the growth and differentiation of neurons and promotes long-term potentiation, a form of synaptic plasticity widely considered a cellular model of long-term memory formation. 5 In animal models, BDNF has been shown to modulate the number and shape of dendritic spines in mature hippocampal neurons, potentially leading to increased synaptic efficacy, the “hallmark of long-term potentiation.” 6 , 7 BDNF is additionally thought to play a role in reinforcing neural plasticity, by consolidating connections between neurons to promote synchronized activity. 5 Mind–body meditation practices may have a profound effect on memory and attention and are associated with increased cortical thickness, possibly through BDNF activation, increased BDNF circulation, and subsequent neuronal growth. 4 , 8 – 11 These findings indicate that meditation may serve as a BDNF promoter and may have a powerful effect on learning potential. 12
Cortisol, a hormone commonly associated with stress, has likewise been found to play an important role in learning and memory, with elevations having both positive short-term and negative long-term effects on cognitive performance. 13 Cortisol binds to high-affinity hippocampal receptors, and even a slight increase can enhance long-term potentiation 14 ; however, long-term cortisol caused by prolonged stress can disconnect neural networks and inhibit neurogenesis. 15 Meditation has also been implicated in cortisol reduction in high-stress populations, 16 indicating another potential pathway for an effect on memory and cognition though more research is needed for definitive conclusions.
This pilot study aimed to collect preliminary data evaluating the relationship between meditation, circulating biomarker levels, and cognitive function through an online brain-training program. An additional aim of the study was to determine whether a difference in BDNF and cortisol could be measured after a single meditation session as previous studies have looked at longer-term effects. Finally, this study also aimed to determine whether there were differences with respect to BDNF and cortisol in experienced meditators versus inexperienced meditators, as previous studies have compared meditation versus no meditation.
Lumos Labs’ Lumosity was identified as an accessible at-home tool, which has been used to measure performance and learning ability related to lifestyle factors, brain injury, and age. 17 We assessed changes in circulating levels of BDNF, cortisol, and Lumosity scores following one-time seated Qigong meditation intervention in a population of experienced meditators and meditation-naive individuals. We hypothesized that experienced meditators would exhibit higher mean baseline and post-intervention BDNF levels, exhibit lower mean baseline and post-intervention serum cortisol levels, and exhibit higher baseline scores and a greater magnitude in score change after intervention on the Lumosity Cognitive Assessment when compared to inexperienced meditators. Additionally, we pose that if a single meditation session and/or experience with meditation can be associated with higher BDNF and lower cortisol, this could suggest a potential mechanism for future studies related to neuroplastic changes and learning with implications for neurodegenerative diseases and conditions associated with low BDNF.
METHODS
STUDY DESIGN, RECRUITMENT, AND PROCEDURES
We conducted a single-blind, non-randomized, two-group pilot study in healthy individuals following meditation to (1) examine changes in circulating BDNF; (2) examine changes in circulating cortisol; and (3) explore differences in novel cognitive performance scores. Statistical analyses were blinded to group allocation. All study procedures were conducted at the Helfgott Research Institute in Portland, OR. The protocol was approved by the Institutional Review Board (IRB) at the National University of Natural Medicine (NUNM IRB #09182014B) and conducted according to the principles of the Declaration of Helsinki. Participants provided written consent for all procedures associated with the study.
Recruitment for study participation was primarily through physical and digital flyers. Participants were initially screened by telephone to determine eligibility. Upon eligibility, participants were invited to an in-person visit and provided the consent form for their review.
At the study visit, participants were asked to perform the cognitive performance test via three “Brain Games” by Lumosity (Tidal Treasures, Speed Match, and Memory Match to assess short-term recall, information processing, and working memory, respectively). The scores were recorded after each game and participants immediately received a blood draw to obtain baseline specimens for circulating BDNF and cortisol. Following this, participants were provided meditation instructions. After review, participants went into a quiet room without supervision and performed 30 minutes of Qigong meditation followed by a signal ending the meditation, as described below. The participant received a post-intervention blood draw for specimen collection and repeated the same three Lumosity Brain Games. The scores were recorded a second time.
The primary endpoints for the trial were circulating levels of BDNF and cortisol prior to and following meditation. An exploratory endpoint for the trial was changes in cognitive performance scores via Lumosity.
PARTICIPANT ELIGIBILITY AND ALLOCATION
Participants were prospectively enrolled and allocated to one of two groups according to self-reported level of experience with meditation of any kind: ?3 years of meditation practice and/or >4 days/week working with a meditation group or no meditation history within 2 years. Those eligible to participate were people aged 18–60, able to speak, read, and understand English, and able to provide written consent to participate. Participants were excluded if they reported a history of Alzheimer’s disease, Parkinson’s disease, schizophrenia, depression, epilepsy, chronic obstructive pulmonary disease or other restrictive airway disease, prior use of the Lumosity platform, or exercise within 12 hours of the intervention as these have been shown to decrease BDNF levels compared to an otherwise healthy population. Individuals with chronic obstructive pulmonary disease (COPD) or other pulmonary disease were excluded due to possible challenges with deep breathing during meditation.
QUALITY CONTROL
We performed a pilot experiment to determine BDNF degradation with overnight refrigeration by comparing serial dilutions of recombinant BDNF protein and a sample from the following day using the BDNF Emax Immunoassay System and subsequent plate analysis at 450 nm on a MAXline microplate reader using Softmax Pro 4.8 software. BDNF was unstable during refrigerated storage; therefore, all serum samples were stored at ?80°C after collection to minimize degradation prior to analysis. We also calibrated the appropriate dilution for participants’ serum samples against the enzyme-linked immunosorbent assay (ELISA) standard curve, which suggested that a 1:100 serum dilution was optimal for measuring BDNF in this study.
SPECIMEN COLLECTION
Blood draws were administered according to NUNM’s protocol for standard venipuncture procedures. Blood collection at each time point consisted of a venous blood draw into a single serum separation tube (SST) (Becton Dickinson, Franklin Lakes, NJ; catalog #367988). One 8.5 mL vial of blood was drawn from each participant at each blood draw, for a total of 17 mL for the entire study. Serum samples were labeled with participant ID’s and analyses of samples were blinded to participants’ previous meditation experience.
Following each blood draw into a serum separator tube, the tube was inverted and allowed to clot at room temperature for at least 30 minutes but not more than 2 hours from the time of draw. Tubes were centrifuged for 10 minutes at 1200 rpm and subsequently divided into 500 mL aliquots, labeled with the participant’s ID number, and stored at ?80°C until analysis to prevent possible degradation as demonstrated in a pilot analysis at conventional refrigeration temperatures.
INTERVENTION
The meditation script was adapted from The Shaolin Grandmasters’ Text: History, Philosophy, and Gung Fu of Shaolin Ch’an (see Appendix 1 for original text and adapted script). Participants were instructed via script (provided verbally and by physical copy) on seated Qigong meditation and asked to meditate alone for 30 minutes with a chime indicator noting the start and end time of the meditation sequence.
OUTCOME ANALYSES
Mean BDNF, cortisol, and cognitive performance scores were compared between groups at baseline using two-sample t -tests. In the case of non-normal distributions, a non-parametric Mann–Whitney test was used. Pre–post changes in all outcomes were analyzed by linear mixed analysis of variance (ANOVA) with meditation group and time as factors. Significant results were further analyzed by the paired t -test for pre–post changes in all participants and two-sample t -test comparing pre–post changes between groups. Pre-/post intervention means changes in Lumosity game scores were compared for each separate game, both within and between groups.
Power and sample size
Sample size was determined for mean change in serum BDNF from before to after meditation among all participants. Based on previous literature, the estimated standard deviation of BDNF at baseline was projected to be approximately 7 ng/mL. 18 Using ?=0.05 and assuming a pre–post correlation of r=0.8, 20 participants were required to achieve 80% power to detect a mean change of 3 ng/mL of BDNF by the paired t -test.
BDNF and cortisol
Levels of BDNF were analyzed in triplicate at a 1:100 serum dilution by enzyme-linked immunosorbent assay (Emax Immunoassay System, Promega, Madison, WI, #G7610). Levels of cortisol were analyzed off-site (ZRT Laboratories, Beaverton, OR). Following each ELISA, mean triplicate standard curve absorbance values were plotted against each standard curve concentration. A trend line was fitted to the standard curve points using Microsoft Excel to calculate the BDNF concentration of each sample from the average absorbance value of the sample. As a measure of goodness of fit, an r 2 value of >0.996 was obtained for all standard curve trend lines. BDNF concentrations were multiplied by the dilution factor used in ELISA to generate the final serum BDNF concentration for each participant.
Cognitive assessment
As an exploratory outcome, participants performed three Lumosity Brain Games prior to the intervention. The results from each game were recorded as a raw value and established as baseline scores. Following the 30-minute meditation, participants performed the same three Brain Games. These results were also recorded on a collection form and compared between groups to baseline by two-sided t -tests.
RESULTS
This small pilot study of 14 participants examined changes in BDNF, cortisol, and cognition with meditation. Seven experienced meditators and seven inexperienced meditators were enrolled. Participants completed a Luminosity cognitive test and then underwent a blood draw. They then completed a Qigong seated meditation for 30 minutes. Following the meditation, they were administered another Luminosity cognitive test and another blood draw for comparison. Because the entire study took place in a single visit, there were no dropouts ( Figure 1 ). While this pilot study was not large enough to achieve statistical significance, the data could serve as preliminary data for a larger clinical trial.
- Figure 1: -
Study design.
Both groups were similar with respect to age; mean age for inexperienced meditators was 35 years, and for meditators, it was 34 ( Table 1 ). Ages ranged from 25 to 51 years (SD±9.4). Mean weight among participants was 165 lbs (±40), with a range from 125 to 250 lbs.
- Table 1: -
Demographics.
- - - - - - - - - - - - - - - - -
| - | Experienced meditators ( n =7) | Inexperienced meditators ( n =7) |
|---|---|---|
| Age (SD) | 33 years (±9.4) | 35 years (±9.4) |
| Gender | Male ( n =3) | Male ( n =2) |
| Female ( n =4) | Female ( n =5) | |
| Mean baseline BDNF (SD) | 29.9 (±6) ng/mL | 30.5 (±5) ng/mL |
| Mean baseline cortisol (SD) | 10.0 (±2.7) ?g/dL | 9.8 (±1.8) ?g/dL |
| Mean baseline Tidal Treasures Score (SD) | 23,014.3 (8085.0) | 23,371.4 (5425.0) |
| Mean baseline Speed Match Score (SD) | 18,485.7 (2237.0) | 15,792.9 (7234.6) |
| Mean baseline Memory Match Score (SD) | 6585.7 (3425.9) | 9371.4 (5106.1) |
-
This table reflects baseline demographics of the two groups.
The groups differed in their experience with meditation. Mean years of meditation among experienced meditators was 12.5 years (±8.9); mean days per week of meditation among experienced meditators was 5.7 (±1.7) days. Mean minutes per meditation for experienced meditators was 33 (±17) minutes. In contrast, inexperienced meditators were recruited specifically if they had not meditated regularly for the past two years. Inexperienced meditators had only 4.6 (±5.4) years of experience. Inexperienced meditators meditated only 1 (±0.000) day and mean minutes per meditation session for inexperienced meditators was 14 (±22).
The mean baseline BDNF level in the inexperienced meditator group was 29.1 (±5) ng/mL, while the mean baseline BDNF in experienced meditators was 29.9 (±6) ng/mL ( Table 1 ). After meditation, inexperienced meditators increased overall to a mean BDNF level of 30.5 (±5) ng/mL and meditators decreased to a mean BDNF level of 29.3 (±5) ng/mL ( Figure 2 ). The difference between experienced and inexperienced meditators’ baseline BDNF was not statistically significant by independent sample t -test ( P =0.783). There was also no statistically significant difference between groups after meditation for BDNF ( P =0.661) ( Table 2 ). ANOVA between all participants showed no significant difference between the change of BDNF from pre- to post-meditation [ F (1,12)=18.3, P =0.082, r 2 =0.230, 95% CI=1.1, 20]. A linear regression indicated no statistical significance of variable effect on baseline BDNF [ F (8,13)=2.6, P =0.113].
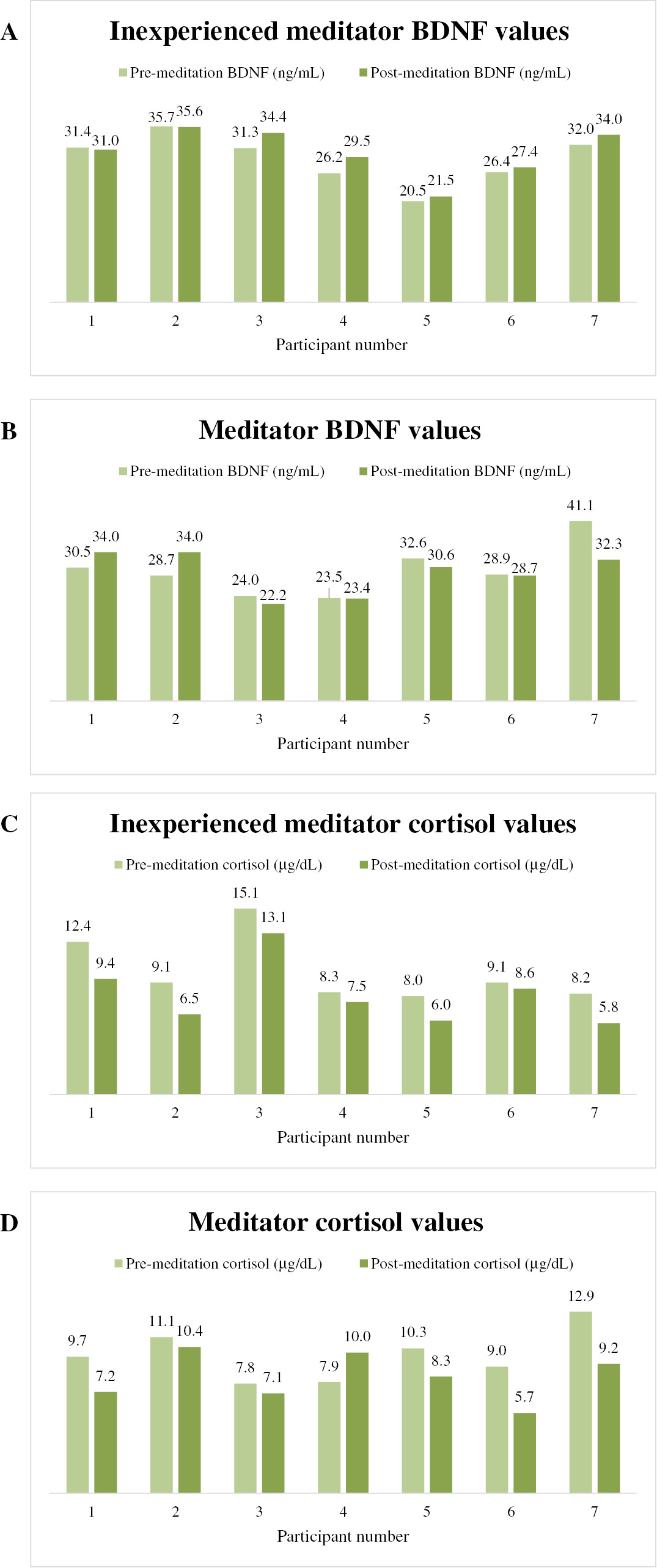
- Figure 2: -
Individual variability in BDNF and cortisol pre- and post-meditation.
BDNF was measured by ELISA in inexperienced meditators (A) and experienced meditators (B). Cortisol was measured in inexperienced meditators (C) and experienced meditators (D).
- Table 2: -
Changes in BDNF, cortisol, and test scores following intervention.
- - - - - - - - - - - - - - - -
| - | Experienced meditators ( n =7) | Inexperienced meditators ( n =7) | P -value |
|---|---|---|---|
| Mean BDNF change (SD) | 0.4 (±3.4) ng/mL | 0.661 a | |
| Mean cortisol change (SD) | ?1.7 (±1.5) ?g/dL | <0.001 a | |
| Mean Tidal Treasures Score Change (SD) | 57.1 (3.0) | 5528.6 (10,929.4) | 0.380 b |
| Mean Baseline Speed Match Score Change (SD) | 200.0 (3067.4) | 2992.9 (3490.5) | 0.138 b |
| Mean Memory Match Score Change (SD) | 1278.6 (3391.8) | 2171.4 (5293.9) | 0.613 b |
-
This table reflects changes in BDNF and cortisol levels in all participants and changes in Lumosity scores between groups.
a Paired sample t -test was used to assess differences in all participants.
b Two-sample t -test was used to assess differences in mean change between groups. P -values <0.05 were considered statistically significant.
Individuals responded to meditation differently. Since we had a small number of study participants, we could look at the changes in each person. BDNF levels were more likely to increase with inexperienced meditators. Five inexperienced meditators experienced an increase in BDNF, and two did not. In contrast, only two meditators experienced an increase in BDNF, and five experienced a decrease in BDNF ( Figure 2 ). The odds of increasing BDNF from the act of meditation was 0.16 times higher in the inexperienced meditator group compared to the experienced meditator group.
Qigong meditation reduced cortisol in both inexperienced meditators and experienced meditators ( Figure 2 ). The mean baseline cortisol level in inexperienced meditators was 10.0 (±3) ?g/dL compared to 9.8 (±2) in meditators. Mean cortisol after meditation in inexperienced meditators was 8.1 (±3) ?g/dL and 8.3 (±2) ?g/dL in meditators. There was no statistically significant difference between experienced and inexperienced meditators’ baseline cortisol levels ( P =0.864) or post-Qigong ( P =0.904). A paired sample t -test indicated a statistically significant reduction in cortisol among all participants after meditation ( Table 2 ; n =14, P <0.001). Pearson correlation indicates strong positive correlation between BDNF and cortisol before meditation ( P =0.29).
After meditation, the mean change in Lumosity Game 1 (Tidal Treasures) score (point difference from pre- to post-meditation scores) for inexperienced meditators was 57 points; meditators showed a mean change of 5529 points; for Game 2 (Speed Match), mean score for inexperienced meditators was 200 points and 2993 points for meditators; for Game 3 (Memory Match), mean score for inexperienced meditators was 907 points and 2171 points for meditators ( Figure 3 ). There was no statistically significant difference between change in Lumosity Brain Games cognitive assessment scores, Game 1 ( P =0.380), Game 2 ( P =0.138), or Game 3 ( P =0.613) from pre- to post-meditation scores, likely due to the small sample size ( Table 2 ).
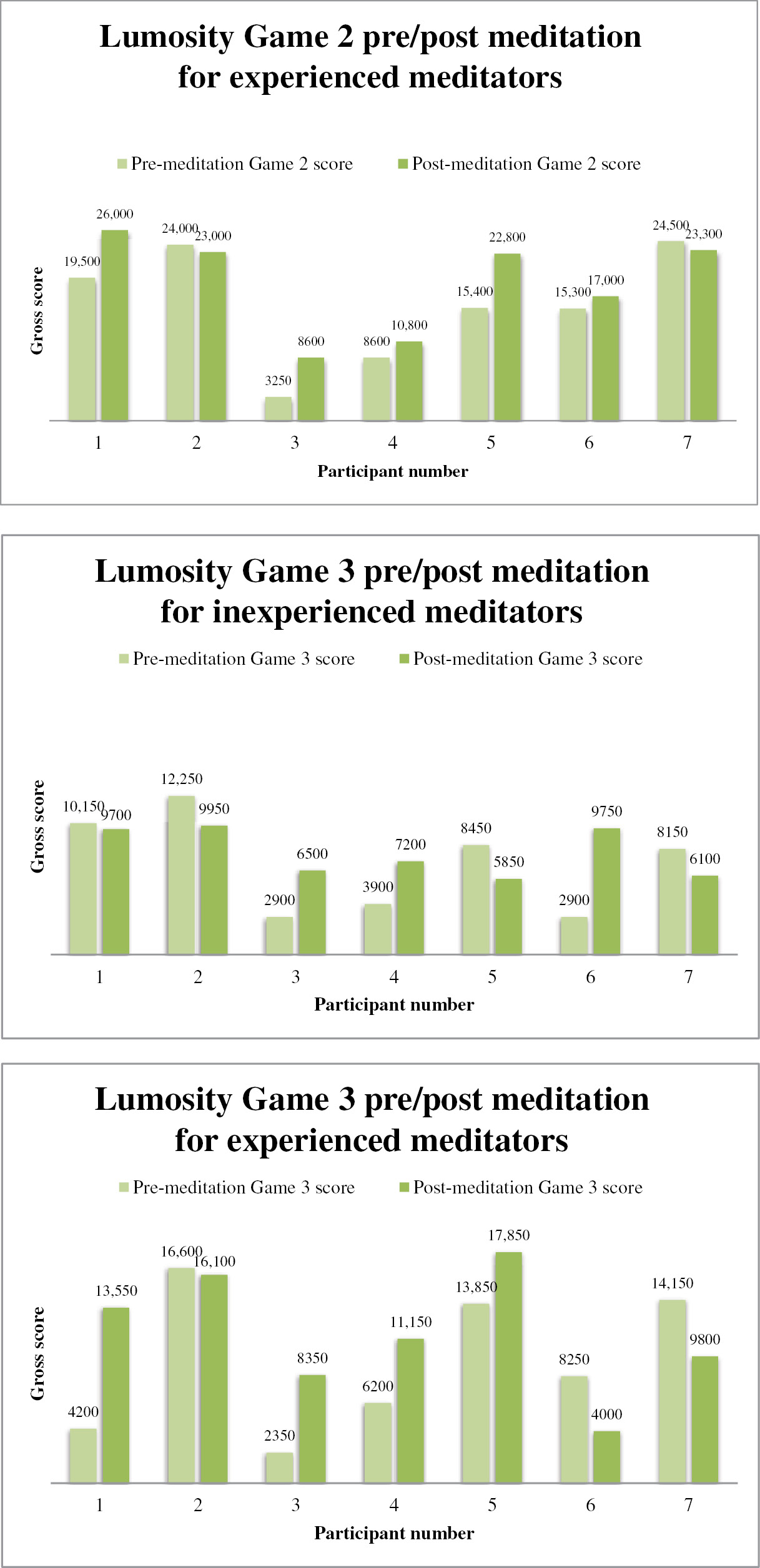
- Figure 3: -
Individual variability in Lumosity scores pre- and post-meditation.
Gross scores for three Lumosity were noted in inexperienced meditators and experienced meditators before and after intervention.
DISCUSSION
This study looked for changes in BDNF after a single meditation sitting as the primary outcome. Previous studies have demonstrated changes in BDNF after a 3-month yoga and meditation retreat with a correlated decreased in anxiety levels. 11 A recent meta-analysis also showed that mindfulness-based meditation can increase BDNF. 12 In this meta-analysis, the control group experienced no mindfulness intervention. This pilot study aimed to determine whether a difference in BDNF and cortisol could be measured after a single meditation session and to determine whether there were between group differences with respect to BDNF and cortisol after meditation.
In our study, both experienced meditators and inexperienced meditators received a meditation intervention, and we observed a decrease in cortisol as a secondary outcome in both groups. Decrease in cortisol is often associated with decreased stress and anxiety.
We chose to compare people with meditation experience to those without meditation experience as we were curious as to whether a “ceiling effect” would be observed (i.e.,would those who were experienced meditators already produce a high level of BDNF such that we could not see a difference with meditation?). In fact, baseline BDNF levels were similar for experienced and inexperienced meditators. Our small sample demonstrated a mean increase of BDNF in inexperienced meditators and decrease in experienced meditators, though the difference was not significant. These results are likely due to normal variability and any trend may be explored more thoroughly with a sufficiently large sample size.
The act of meditation is known to increase the “focus” and “attention” areas of the brain. For experienced meditators, mean Lumosity scores improved in all games after Qigong when compared to inexperienced meditators. This could account for the meditators greater average scores on the Lumosity brain games, as a more consistent practice of meditation has been shown to increase brain gyrification. 10 With no prior validation to these tools, this outcome was exploratory in nature in this intervention. It is unclear how well the performance on Lumosity measures might extend to gross structural changes in the brain such as the type of neuronal growth that has been associated with BDNF and may be a potential aim for future trials.
There were multiple limitations to this study. First, as our small sample size did not meet outlined power projections, notably for mean change in BDNF, no conclusive statements can be generated regarding the relationship of a single seated meditation to circulating BDNF and cortisol. In retrospect, the group allocation criteria were ambiguous in that we did not specifically exclude other mind–body practices with both exercise and meditation components, such as yoga. Experienced meditators also reported varying length and frequency of meditation, possibly contributing to increased heterogeneity within the small group. Future studies would benefit by taking this into consideration.
Second, the act of a single 30-minute meditation may have proved difficult for participants regardless of group allocation. Our study did not assess a subjective level of success in meditation, nor did we record meditation length. Finally, the diurnal patterns of BDNF and cortisol circulation were a potential confounder for this study. As circulating BDNF levels peak around 8 a.m., this may have been a “ceiling effect” for how much a participant’s BDNF could have risen. 19 Similarly, a natural post-awakening decline in cortisol may have been an influencer on the pattern observed in this study. Due to lack of consistency in study visit timing, it is unclear how our study may have been affected by these natural rhythms.
CONCLUSION
This pilot study aimed to assess the effect of Qigong meditation on circulating levels of BDNF and cortisol, as well as potential effect on cognitive performance through a novel assessment tool, in a population with mixed levels of experience and familiarity with meditation. We found no statistical evidence of an effect on baseline or post-meditation BDNF levels or cognitive performance. We observed a reduction in circulating levels of cortisol regardless of experience as well as a trend toward inverse changes in BDNF levels according to experience with meditation. This pilot study was underpowered due to a small sample size, though the results suggest a reduction in cortisol may be observable through meditation. It also suggested that BDNF changes may be more observable in inexperienced meditators and should be considered for exploration in larger studies.
References
- Black DS, Slavich GM. Mindfulness meditation and the immune system: a systematic review of randomized controlled trials. Ann N Y Acad Sci. 2016;1373(1):13–24.
- Gotink RA, Meijboom R, Vernooij MW, et al. 8-Week mindfulness based stress reduction induces brain changes similar to traditional long-term meditation practice: a systematic review. Brain Cogn. 2016;108:32–41.
- Zagrebelsky M, Holz A, Dechant G, et al. The p75 neurotrophin receptor negatively modulates dendrite complexity and spine density in hippocampal neurons. J Neurosci. 2005;25(43):9989–99.
- Jahnke R, Larkey L, Rogers C, et al. A comprehensive review of health benefits of Qigong and Tai Chi. Am J Health Promot. 2010;24(6):e1–25.
- Noble EE, Billington CJ, Kotz CM, et al. The lighter side of BDNF. Am J Physiol Regul Integr Comp Physiol. 2011;300(5):R1053–69.
- Olson AK, Eadie BD, Ernst C, Christie BR. Environmental enrichment and voluntary exercise massively increase neurogenesis in the adult hippocampus via dissociable pathways. Hippocampus. 2006;16(3):250–60.
- Bosch M, Castro J, Saneyoshi T, et al. Structural and molecular remodeling of dendritic spine substructures during long-term potentiation. Neuron. 2014;82(2):444–59.
- Chan KL, Tong KY, Yip SP. Relationship of serum brainderived neurotrophic factor (BDNF) and health-related lifestyle in healthy human subjects. Neurosci Lett. 2008;447(2–3):124–8.
- Kim JJ, Song EY, Kosten TA. Stress effects in the hippocampus: synaptic plasticity and memory. Stress. 2006;9(1):1–11.
- Kang DH, Jo HJ, Jung WH, et al. The effect of meditation on brain structure: cortical thickness mapping and diffusion tensor imaging. Soc Cogn Affect Neurosci. 2013;8(1):27–33.
- Cahn BR, Goodman MS, Peterson CT, et al. Yoga, meditation and mind-body health: increased BDNF, cortisol awakening response, and altered inflammatory marker expression after a 3-month yoga and meditation retreat. Front Hum Neurosci. 2017;11:315.
- Gomutbutra P, Yingchankul N, Chattipakorn N, et al. The effect of mindfulness-based intervention on brainderived neurotrophic factor (BDNF): a systematic review and meta-analysis of controlled trials. Front Psychol. 2020;11:2209.
- Lupien SJ, de Leon M, de Santi S, et al. Cortisol levels during human aging predict hippocampal atrophy and memory deficits. Nat Neurosci. 1998;1(1):69–73.
- Sapolsky RM, Krey LC, McEwen BS. The neuroendocrinology of stress and aging: the glucocorticoid cascade hypothesis. Endocr Rev. 1986;7(3):284–301.
- McEwen BS, Sapolsky RM. Stress and cognitive function. Curr Opin Neurobiol. 1995;5(2):205–16.
- Koncz A, Demetrovics Z, Takacs ZK. Meditation interventions efficiently reduce cortisol levels of atrisk samples: a meta-analysis. Health Psychol Rev. 2021;15(1):56–84.
- Zickefoose S, Hux K, Brown J, Wulf K. Let the games begin: a preliminary study using attention process training-3 and Lumosity™ brain games to remediate attention deficits following traumatic brain injury. Brain Inj. 2013;27(6):707–16.
- Goda A, Ohgi S, Kinpara K, et al. Changes in serum BDNF levels associated with moderate-intensity exercise in healthy young Japanese men. Springerplus. 2013;2:678.
- Choi SW, Bhang S, Ahn JH. Diurnal variation and gender differences of plasma brain-derived neurotrophic factor in healthy human subjects. Psychiatry Res. 2011;186(2–3):427–30.