Abstract
OBJECTIVE:
To review the current literature regarding vitamin D insufficiency and supplementation in major illnesses.
DESIGN AND METHODS:
We reviewed Pubmed-indexed, English language manuscripts from January, 2003 to June, 2012 using search terms related to vitamin D, all-cause mortality, cardiovascular disease, pulmonary disease, diabetes mellitus, and cancer.
OUTCOME MEASURES:
Incidence of disease, risk ratios associated with 25-hydroxyvitamin D [25(OH)D] levels, and/or vitamin D supplementation schedules were documented.
RESULTS:
Although 25(OH)D levels ≥20 ng/mL were often associated with improved health outcomes, evidence suggests that 25(OH)D levels ≥30 ng/mL may confer additional health benefits.
CONCLUSIONS:
Based on the available evidence, vitamin D supplementation to restore 25(OH)D levels within a range of 30-50 ng/mL is reasonable in order to optimize potential benefits and minimize potential risks. This, of course, should be considered in the context of individual patient needs and co-morbidities.
Introduction
Vitamin D is an important hormone, historically considered a key requirement only for musculoskeletal development and function. However, as the prevalence of low vitamin D status has increased dramatically in the general population of the United States, its pleotropic effects have recently garnered significant attention. Growing recognition of the association between vitamin D insufficiency and increased risk of a significant number of major public health challenges has stimulated significant research on the topic. Taken on aggregate, studies - though varying in their specific outcomes - suggest that vitamin D supplementation may attenuate the risk of various diseases and may also reduce all-cause mortality. In our current review of the literature, we will address some critical background information related to the measurement of vitamin D status, the appropriateness of 25-hydroxyvitamin D [25(OH)D] as a biomarker for disease, and the associations between vitamin D status as well as all-cause mortality, cardiovascular disease, pulmonary ailments, diabetes mellitus, and cancer. We will also review the current evidence related to dosing of vitamin D supplements to achieve “therapeutic” levels of 25(OH)D.
MEASURING VITAMIN D LEVELS:
Vitamin D is a 27-carbon secosteroid, yet it is unlike most other hormones. Differences in source (endogenous vs. exogenous pre-hormone), extensive need for tissue modification (skin vs. liver vs. kidney), an active intermediary pro-hormone [25(OH)D], and a critical set of modulators (parathyroid hormone [PTH], calcium, phosphorus, and fibroblast growth factor-23 [FGF-23]) add to the complexity of vitamin D regulation. Taken together, these factors complicate the direct measurement of vitamin D, as well as which parameter would best reflect overall vitamin D status.
Upon exposure to ultraviolet B irradiation, endogenous synthesis of vitamin D3 starts with a photochemical reaction in the epidermis (Figure 1). 7-dihydrocholesterol (pro-vitamin D) is converted to pre-vitamin D3, which in turn is transformed to vitamin D3 by isomerization through a temperature-dependent reaction. Alternatively, vitamin D can be supplied exogenously as a nutrient. Dietary sources of vitamin D3 (cholecalciferol) include fatty fish, enriched dairy products, and egg yolk. Plant materials also contribute to vitamin D intake, but this is in the form of vitamin D2 (ergocalciferol). Structurally, vitamin D3 and D2 differ in their side chains. Although their metabolic pathways are identical and both may contribute to vitamin D adequacy, vitamin D3 appears be more efficiently metabolized than vitamin D2.
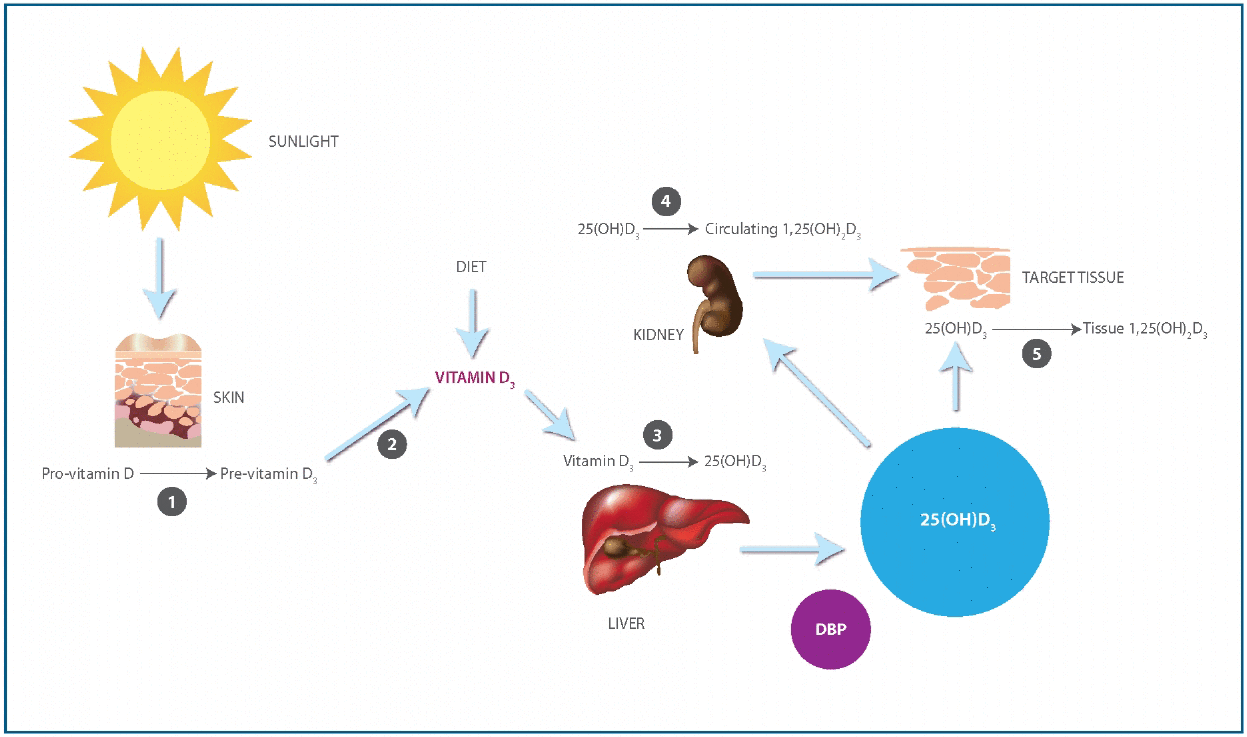
(1) Reaction catalyzed by UVB (290-310 mm). (2) Isomerization reaction catalyzed by heat. (3) Reaction catalyzed by 25-hydroxylase. (4) Reaction catalyzed by renal 1-α-hydroxylase. (5). Reaction catalyzed by tissue 1-α-hydroxylase. 25(OH)D3: 25-Hydroxyvitamin D3. DBP: Vitamin D binding protein. 1,25(OH)2D3: 1,25-Dihydroxyvitamin D3.
Vitamin D traverses the systemic circulation after binding to vitamin D binding protein (DBP) and is hydroxylated in the liver to 25(OH)D. A strong regulation of this step does not exist and there is no signific ant storage of 25(OH)D in the liver. 25(OH)D is rapidly released by the liver into the circulation, where under normal circumstances, it exhibits a biological half-life of approximately 12-19 days. In the kidney, 25(OH)D is enzymatically converted to the vitamin D hormone calcitriol (1,25-dihydroxyvitamin D [1,25(OH)2D]), which is the most biologically active metabolite of the vitamin D synthesis pathway. This final step is rigidly controlled by the stimulus of PTH, inhibition by FGF-23, and circulating levels of calcium, phosphorus, and 1,25(OH)2D itself. These mechanisms are known to be highly efficient except during renal failure, when 1-α-hydroxylation is impaired despite high levels of PTH. Serum 25(OH)D levels are approximately 500-1000 times higher than 1,25(OH)2D levels, and both are predominantly protein bound in circulation. Indeed, only 0.03% of 25(OH)D is free, with close to 88% bound to DBP and the remainder to albumin.
Serum 25(OH)D levels reflect overall vitamin D contact from diet and sunlight exposure. In general, there is agreement that, under normal circumstances, the serum 25(OH)D level - free and bound, including both 25(OH)D3 and 25(OH)D2 - is the best indicator to define vitamin D status. This is certainly unusual in the sense that a metabolite one step removed from the most biologically active form is used to assess adequacy. Nonetheless, 25(OH)D is the most abundant vitamin D metabolite and its relative stability in the systemic circulation makes it a good indicator of vitamin D stores in the general population. On the other hand, 1,25(OH)2D is present in picomolar concentrations and, because it is tightly regulated, the concentration can remain normal or even be elevated, despite evidence of deficiency. Whereas, the half-life of serum 25(OH)D is generally 2-3 weeks, that of 1,25(OH)2D is only a few hours. Furthermore, measurement of 1,25(OH)2D may be confounded by the greater technical difficulty in performing the assay (subject to greater error) and that conditions such as renal insufficiency or advanced aging reduce 1-α- hydroxylase activity, which is a major cause of low levels of 1,25(OH)2D independent of vitamin D stores.
VITAMIN D LEVELS AS A BIOMARKER:
The role of 25(OH)D levels as a biomarker for disease is promising, but not uniformly accepted. Widespread utilization of thresholds to define disease risk has led to multiple issues from both a clinical and research perspective. To date, there is no clear consensus about the optimal definitions of either vitamin D deficiency or insufficiency. While there is a strong interest to define the optimal vitamin D status for health, diverse cut points for serum levels of 25(OH)D have been suggested, ranging from 16 to 48 ng/ml. This uncertainty likely originates from the lack of standardized vitamin D assay methodologies and differences in the measured functional endpoints used by various investigators, which arise from the classic and non-classic effects of vitamin D.
The classic function of vitamin D is the control of extracellular calcium metabolism by regulating absorption in epithelia involved in calcium transport. Consequently, the traditional “low normal” level for serum 25(OH)D was 10 ng/mL, as this threshold had the advantage of high specificity for rickets and osteomalacia. Since low vitamin D status stimulates PTH secretion to increase intestinal calcium absorption and bone resorption to maintain calcium balance, it has been proposed that vitamin D sufficiency be described as the concentration of 25(OH)D which achieves maximal PTH suppression. In this regard, vitamin D sufficiency is defined by a serum 25(OH)D of ≥30 ng/mL. Based on studies on fracture prevention, most investigators have adopted the definition of vitamin D insufficiency as a serum 25(OH)D concentration of <30 ng/mL and deficiency as <20 ng/mL. However, in a somewhat controversial 2011 report, the Institute of Medicine (IOM) defined vitamin D adequacy as serum 25(OH)D levels between 20-50 ng/mL, based on an estimate that serum 25(OH)D levels of ≥20 ng/mL would protect 97.5% of the healthy population from skeletal disorders such as osteoporosis and osteomalacia and the potential higher risk of vitamin D toxicity at 25(OH)D levels >50 ng/mL.
The non-classic function of vitamin D includes regulation of cell proliferation and differentiation, regulation of hormone secretion, and the regulation of immune function. These effects take place on a cellular level and are directly dependent on 25(OH)D levels. In fact, cells of the neuromuscular, cardiovascular, endocrine, and immune system express the vitamin D receptor (VDR). Furthermore, most of these cells express the 25(OH)D-1-α-hydroxylase, to produce 1,25(OH)2D for autocrine and paracrine use within the target cell itself. The discovery of VDRs in activated immune cells has particularly stimulated research into the role of vitamin D in immune function. It is now recognized that vitamin D plays a critical role in the regulation of the innate and the adaptive immune systems. Therefore, vitamin D insufficiency is thought to be a mechanism underlying a range of inflammatory, autoimmune, and infective conditions. 1,25(OH)2D inhibits adaptive immunity by attenuating the proliferation and differentiation of both T and B lymphocytes, which is thought to ameliorate the severity of inflammatory and autoimmune diseases. In contrast to its inhibitory role in adaptive immunity, 1,25(OD)2D is a potent activator of the innate immune system. Innate immunity represents the first line of defense against microbial invasion and constitutes both epithelial and mucosal cells, as well as polymorphonuclear leukocytes, monocytes, and macrophages. The central mechanism underlying microbial eradication is the activation of toll like receptors in the host cell, which induces formation of potent antimicrobial peptides such as cathelicidin. Macrophages and epithelial cells respond to both circulating and local 1,25(OH)2D synthesized by 1-α-hydroxylase activity on 25(OH)D. Recent evidence indicates that a positive correlation exists between cathelicidin concentrations and 25(OH)D levels ≤32 ng/mL. This suggests that serum levels of 25(OH)D >30 ng/mL might be necessary for vitamin D to optimally exert its non-classical effects.
ASSOCIATIONS BETWEEN VITAMIN D AND DISEASE
Methods: We performed a targeted literature search through the National Library of Medicine search engine (Pubmed - http:www.ncbi.nlm.nih.gov). Published manuscripts in the English language spanning the period January, 2003 to June, 2012 were reviewed. Various combinations of the following search terms were used to identify potentially suitable manuscripts for review: ‘vitamin D’, ‘25(OH)D’, ’25-hydroxyvitamin D’, ‘all-cause mortality’, ‘mortality’, ‘cardiovascular’, ‘pulmonary’, ‘diabetes’, and ‘cancer’.
Vitamin D and All-cause Mortality:
On prospective evaluation of more that 3000 patients, 25(OH)D levels ≤20 ng/mL were associated with an almost 2-fold increased risk of all-cause mortality compared to patients with 25(OH)D levels >30 ng/mL. Moreover, retrospective data analysis from more than 13,000 adults in the National Health and Nutrition Examination Survey (NHANES) III suggested that individuals with 25(OH)D levels <17.8 ng/mL were likely to have a 26% increased risk of mortality compared to individuals with 25(OH)D >32.1 ng/mL. Another study on the same NHANES III data observed a potential 5% reduction in the risk of all-cause mortality for every 4ng/mL increase in 25(OH)D levels between 0 ng/mL (extrapolation) and 48 ng/mL. All-cause mortality in subjects who participated in randomized trials testing the impact of vitamin D supplementation on any health condition have also been examined. In one report of 18 independent randomized controlled trials (RCTs), daily vitamin D supplementation (ergocalciferol or cholecalciferol) in usual doses (400-800 IU) was associated with a 7% decrease in mortality risk when compared to controls. In a larger meta-analysis of 50 independent RCTs, daily vitamin D supplementation (cholecalciferol, ergocalciferol, alfacalcidiol, or calcitriol) in usual doses was associated with a 3% decrease in mortality risk when compared to controls. In a subgroup analysis of subjects who received cholecalciferol, a potential 6% reduction in mortality risk was observed. Consequently, intake of ordinary doses of vitamin D supplements seem to be associated with decreases in total mortality rates. In a separate, large study, with approximately 11,000 patients, 25(OH)D levels <30 ng/mL were associated with a greater than 1.5-fold increased risk of all-cause mortality when compared to patients with levels ≥30 ng/mL. Vitamin D supplementation (between 1000 IU/day to 50,000 IU biweekly) on the other hand, was associated with a 60% reduction in the risk of all-cause mortality. Furthermore, it is estimated that if global 25(OH)D levels increased from 21.6 ng/mL to 44 ng/mL, reduction in the risk of all-cause mortality may range from 7.6% for African females to 17.3% for European females. Expected reductions for males are on average 0.6% lower than for females. The estimated increase in life expectancy could be 2 years across all geographical regions. Despite some good evidence to suggest an association between 25(OHD levels, supplementation, and all-cause mortality, future large-scale RCTs using standardized measurement and supplementation protocols will be key to understanding the nature of the relationship between vitamin D and mortality.
Cardiovascular Disease:
In a moderately-sized prospective study with 239 patients undergoing coronary angiography, 25(OH)D levels were shown to have a significant inverse association with the severity of coronary artery stenosis. As such, a large retrospective analysis from the Framingham offspring study, which included more than 1700 participants, confirmed the association between vitamin D levels and cardiovascular events. Individuals with 25(OH)D levels <15 ng/mL had a potential 62% greater risk of incident cardiovascular events when compared to individuals with 25(OH)D levels ≥15 ng/mL. A potential 2-fold increase in the risk of incident cardiovascular events was observed in hypertensive individuals in this cohort. Similarly, a potential 3-fold increase in the risk of incident myocardial infarction (MI) was observed in hypertensive patients in a small retrospective study of 139 patients admitted to the hospital for acute coronary syndrome, where patients with 25(OH)D levels >14 ng/mL were compared to patients with levels ≤14 ng/mL. Furthermore, with over 3000 participants, Dobnig et al. prospectively demonstrated that 25(OH)D levels ≤20 ng/mL were associated with an approximate 2-fold increased risk of cardiovascular mortality compared to patients with 25(OH)D levels >30 ng/mL (34). Moreover, in a much larger retrospective data analysis from more than 13,000 adults in NHANES III, individuals with 25(OH)D levels <10 ng/mL had a potential 1.5-fold increased risk of cardiovascular mortality compared to individuals with 25(OH)D ≥40 ng/mL. Participants with 25(OH)D levels <21 ng/mL had a potential 30% greater risk of hypertension and almost 50% greater risk of hypertriglyceridemia when compared to participants with 25(OH)D ≥37 ng/mL. And although a recent prospective study of over 2000 participants free of cardiovascular disease at baseline demonstrated no association between 25(OH)D levels and overall cardiovascular mortality, a potential 25% increase in the risk of incident myocardial infarction (MI) was observed for every 10 ng/mL decrement in 25(OH)D levels ≤30 ng/mL. In hypertensive patients with type 2 diabetes mellitus, a single dose of 100,000 IU ergocalciferol (n=17) was associated with a 14 mmHg drop in systolic pressure when compared to the placebo group (n=17). And in another small randomized clinical trial of 77 women, treatment with 1000 IU of cholecalciferol over 12 weeks was associated with significant improvements in high-density lipoprotein, apolipoprotein A1, and low-density lipoprotein : apolipoprotein B100 ratio when compared to a placebo group. To date, investigations related to vitamin D-related gene polymorphisms have not resulted in convincing association studies. Furthermore, despite significant evidence that suggests hypovitaminosis D may be associated with poor cardiovascular outcomes, there remains a great need for high-quality RCTs to investigate the effect of vitamin D supplementation on cardiovascular-specific morbidity and mortality.
Respiratory Disease:
The relationship between vitamin D status and tuberculosis (TB) has been studied more extensively than most other pulmonary diseases. A recent meta-analysis of 7 studies estimated that individuals with active TB had a 70% likelihood of significantly lower 25(OH)D levels when compared to similar non-TB infected individuals. In a RCT of 192 patients exposed to TB, subjects treated with a single dose of 100,000 IU of vitamin D2 had a significantly enhanced anti-mycobacterial immune response compared to controls. Similarly, pulmonary TB patients treated with conventional therapy plus 10,000 IU of daily cholecalciferol (n=34) for 6 weeks had a significantly higher sputum conversion rate compared to TB patients treated with conventional therapy alone (n=33). Conversely, a similar trial of 126 patients reported no difference in the global sputum conversion rate when patients received 100,000 IU of cholecalciferol (or placebo) on days 14, 28, and 42 of conventional therapy. Sputum conversion rate was, however, significantly higher in vitamin D supplemented patients with the tt genotype in TaqI of the VDR gene.
Vitamin D status may also affect patients with asthma. Prospective analysis of 54 adults with diagnosed asthma demonstrated a significant inverse relationship between 25(OH)D levels and airway hyper-responsiveness as well as FEV1. In addition, 25(OH)D levels were directly related to the response to glucocorticoid therapy. However, these results could not be duplicated in larger studies in adults, while others demonstrated a stronger association in children. And although a direct association between vitamin D status and risk of asthma has not been reported in large cohorts, a significant association between variations in the VDR gene and asthma has been observed, suggesting are role for genetic susceptibility to play a role in the observed associations in smaller cohort studies.
Seasonal variations in influenza and pneumococcal community acquired pneumonia suggest that vitamin D may play an important role in disease risk. In a prospective analysis of 112 patients hospitalized for community acquired pneumonia, 25(OH)D levels <12 ng/mL upon admission were associated with more than 13-fold increased risk of 30-day mortality when compared to similar patients with 25(OH)D levels ≥12 ng/mL. Furthermore, prospective analysis of 198 healthy adults, during a single fall and winter season, subjects with 25(OH)D levels <38 ng/mL had a potential 2-fold increased risk of viral respiratory illness when compared to subjects with 25(OH)D levels ≥38 ng/mL. In another prospective study of 756 young males followed over a 6 month period, 25(OH)D levels <16 ng/mL were associated with a 63% increased risk of more days missed from work due to upper respiratory illness (URI) when compared to 25(OH)D levels ≥16 ng/mL. Retrospective analysis of the NHANES III data in over 18,000 participants demonstrated that 25(OH)D levels <10 ng/mL were associated with a 36% increased risk of recent URI, while 25(OH)D levels ≥10 to <30 ng/mL were associated with a 24% increased risk, when compared to participants with 25(OH)D levels ≥30 ng/mL. Similarly, in a retrospective analysis of 6789 adult subjects from the Nationwide 1958 British Birth Cohort, when the reference group was set as participants with 25(OH)D levels <10 ng/mL, each 4 ng/mL increase in 25(OH)D levels was associated with a 7% reduction in risk of URI. A RCT of 164 men who received 400 IU of cholecalciferol (or placebo) over a 6-month period demonstrated a potential 30% reduction in the risk of missed working days from URIs. Similarly, in a post hoc analysis of 208 women participating in a 3-year vitamin D trial for osteoporosis, URIs were reported by a significantly less number of participants from the treatment group (up to 2000 IU daily) vs. controls.
A positive correlation between 25(OH)D levels and lung function (forced expired volume in one minute - FEV1 - and/or forced vital capacity - FVC) has been observed in moderate to large-sized studies in adult CF patients and in subjects with chronic obstructive pulmonary disease (COPD). In a prospective study of 414 patients with COPD, 25(OH)D levels <20 ng/mL were significantly associated with greater severity of disease. Moreover, the TT genotype in GC of the DBP gene was shown to be associated with a 2-fold increase in risk for COPD. Another cohort analysis of 79 COPD patients demonstrated a positive correlation between 25(OH)D and exercise capacity. Nonetheless, a RCT of 182 COPD patients receiving 100,000 IU cholecalciferol (or placebo) every 4 weeks over a period of one year did not show a global difference in rates of exacerbation, hospitalization, quality of life, or death. However, in the subset of patients with 25(OH)D levels <10 ng/mL (n=30) an almost 40% potential reduction in risk of COPD exacerbations was observed in association with vitamin D supplementation. Overall, these clinical associations and early trials suggest that vitamin D may be beneficial in patients with various pulmonary diseases, but more importantly highlight the urgent need for further well-designed, high-quality, RCTs.
Diabetes Mellitus:
Epidemiologic data suggests a link between exposure to vitamin D early in life and the development of type 1 diabetes mellitus (DM). A retrospective analysis of over 10,000 adults followed since birth (for approximately 31 years) demonstrated an potential 80% reduction in the risk of developing type 1 DM in individuals who regularly consumed a 2000 IU vitamin D supplement vs. those who consumed lower doses. These findings were reproduced in a meta-analysis of 5 case-controlled studies, which concluded that a 30% reduction in risk for type 1 DM later in life may be associated with regular vitamin D supplementation in infancy. Of note, a dose-response effect was observed, whereby patients taking higher doses of supplements appeared to have a lower risk of disease. Moreover, regression analysis of national registry data from Finland revealed an inverse association between decreasing public health department recommendations for daily vitamin D supplementation over 40 years (1965-2005) and the incidence of type 1 DM during the same time period. Furthermore, a meta-analysis of 57 case-controlled studies demonstrated that the presence of the B allele (BB or Bb) in Bsml of the VDR gene was associated with a 30% greater risk of type 1 DM. However, subgroup analysis revealed the effect was predominantly in patients of Asian decent (where the risk appeared to be almost 2-fold).
The risk of developing type 2 DM may also be related to vitamin D status. On multiple regression analysis of 126 glucose-tolerant adults, a positive association was observed between 25(OH)D levels and insulin sensitivity. In the same study, not only was there a negative association between 25(OH)D levels and observed plasma glucose during oral-glucose-tolerance testing, but also in subjects with baseline 25(OH)D levels <20 ng/mL there was a higher prevalence of components of the metabolic syndrome. Similar associations between 25(OH)D levels, β-cell function, and insulin sensitivity were reproduced in a more recent study involving 150 healthy, glucose-tolerant subjects. Although meta-analysis of 4 observational studies failed to show an overall association between 25(OH)D levels and risk of type 2 DM, after excluding data from non-Hispanic blacks, 25(OH)D levels between 25-38 ng/mL were associated with a 65% reduction in the risk of type 2 DM compared to subjects with 25(OH)D levels between 10-23 ng/mL. In a more recent meta-analysis of 11 prospective studies, 25(OH)D levels >32 ng/mL were associated with a 40% lower risk of type 2 DM compared to 25(OH)D levels <19.6 ng/mL. A prospective cohort study over 4 years, involving 1226 participants from southern Spain, demonstrated that individuals with 25(OH)D >18.5 ng/mL had a potential 80% less risk of type 2 DM when compared to individuals with 25(OH)D ≤18.5 ng/mL. Interestingly, no patient in this cohort with 25(OH)D >30 ng/mL developed type 2 DM. On the other hand, a prospective study of over 10,000 women in the Women’s Health Study did not demonstrate a benefit to low-dose vitamin D supplementation on incident type 2 DM. However, some benefit was observed when vitamin D supplementation was given in concert with calcium in the Nurses’ Health Study. A combined daily intake of >1,200 mg calcium and >800 IU vitamin D was associated with a 33% lower risk of type 2 DM when compared with an intake of <600 mg calcium and 400 IU of vitamin D. Despite a number of small, yet targeted studies to examine the association between vitamin D-related gene polymorphisms and type 2 DM, convincing data is yet to be reported. Taken all together, associations between 25(OH)D and type 1 as well as type DM are undeniable. Yet, there remains a great need for well-designed, high-quality RCTs to determine whether vitamin D supplementation can improve outcomes in type 1 and/or type 2 DM.
Cancer:
Associations between 25(OH)D and outcomes in cancer are likely related to the actions of vitamin D on cell growth and differentiation. Predictions based on cohort data analysis of over 1000 men from the Health Professionals Follow-Up study suggested that over a range of baseline 25(OH)D levels of 9 to 36 ng/mL, a 10 ng/mL increment in 25(OH)D levels would be associated with a 17% reduction in the risk of total cancer incidence and 29% reduction in the risk of total cancer-related mortality. In a subset analysis of only digestive system cancers, the same 10 ng/mL increment in 25(OH)D levels was estimated to result in a 43% reduction in the risk of cancer and a 45% reduction in the risk of cancer-related mortality. Nonetheless, analysis of the NHANES III data from over 16,000 participants failed to demonstrate a relationship between 25(OH)D and total cancer mortality, except in patients with colorectal cancer.
In the colorectal cancer subset from NHANES III, 25(OH)D levels ≥32 ng/mL were associated with a 72% reduction in risk of colorectal cancer-related mortality compared to 25(OH)D levels <20 ng/mL. A meta-analysis of 9 other studies also demonstrated that over a range of clinically applicable values for 25(OH)D, each 10 ng/mL increment in 25(OH)D levels is associated with a 7% reduction in the risk of colorectal cancer. Moreover, a meta-analysis of 5 nested case-control studies demonstrated that 25(OH)D levels ≥33 ng/mL was associated with a 50% reduction in risk of colorectal cancer compared to 25(OH)D levels ≥12 ng/mL. In a more comprehensive meta-analysis of 10 prospective studies, each 100 IU increment in dietary vitamin D consumption (over a range of 39-719 IU) was associated with a 5% reduction in the risk of colorectal cancer. And although pooled data from 2 studies also demonstrated that each 100 IU increment in vitamin D supplementation (over a range of 0-600 IU) was associated with a 7% reduction in the risk of colorectal cancer, a significant inverse association between total vitamin D consumption and colorectal cancer risk could not be detected. Genetic analysis has not demonstrated an association between most vitamin D-related polymorphisms and the risk of colorectal cancer, expect in a single meta-analysis of 8 studies, where the BB genotype in Bsml of the VDR gene was associated with a 40% reduction in the risk of colorectal cancer compared to the bb genotype. However, another meta-analysis of 5 case-controlled studies failed to demonstrate an association between risk of colorectal cancer and polymorphisms in the VDR genes Fokl and Bsml.
In a large prospective analysis of over 30,000 participants from the Women’s Health Study, followed for 10 years, daily consumption of calcium ≥1366 mg and vitamin D ≥548 IU amongst premenopausal women was associated with a 40% reduction in the risk of breast cancer compared to daily consumption of calcium <617 mg and vitamin D <142 IU. A separate RCT in postmenopausal women found significant overall cancer-related benefit associated with calcium and vitamin D consumption. In an analysis of over 1100 postmenopausal women, followed over 4 years, daily consumption of 1500 mg calcium and 1100 IU cholecalciferol was associated with a 60% reduction in the risk of all cancers compared to placebo. Meta-regression analysis of 9 studies found that a 20 ng/mL increase in 25(OH)D over a clinically valid range of baseline values was associated with a 20% reduction in the risk of breast cancer. Similarly, another meta-regression analysis of 10 studies confirmed that a 10 ng/mL increase in 25(OH)D over a clinically valid range of baseline values was associated with a 10% reduction in the risk of breast cancer. In contrast to these findings, a RCT of over 5000 participants (85% female) over a 3-year period did not find a difference in mortality, vascular disease, cancer mortality, or cancer incidence between participants randomized to daily calcium 1000 mg and vitamin D 800 IU vs. placebo. Genetic studies on the association between common vitamin D-related polymorphisms and breast cancer risk have resulted in conflicted reports. While no association was appreciated in women of Chinese decent, pooled data from 6 prospective studies demonstrate that the ff genotype in Fokl of the VDR gene is associated with a 16% increased risk of breast cancer compared to the FF genotype. This association was replicated in a larger meta-analysis of 21case-controlled studies, which also suggested that the results were mostly significant in subjects of European decent. A more recent retrospective analysis of over 1,700 patients and over 1,800 controls in the Canadian province of Ontario demonstrated that the ff genotype in Fokl of the VDR gene is associated with a 30% reduction in the risk of breast cancer. Conversely, the BB genotype in Bsml of the VDR gene was found to be associated with a 25% reduction in risk of advanced breast cancer compared to the bb genotype in one meta-analysis, but this result was not replicated in a larger meta-analysis.
To date, all meta-analyses related to vitamin D and prostate cancer have been unable to detect an association. As such, existing data supports a strong association between vitamin D and colorectal cancer and a clinically relevant association between vitamin D and breast cancer (the heterogeneity of which may be explained by genetic studies). However, more focused, high-quality RCTs are needed to determine whether vitamin D supplementation can improve outcomes.
PUTTING IT TOGETHER FOR CLINICAL PRACTICE
Few recent studies have addressed the issue of optimal daily supplementation regimens. In a small, randomized study of 30 healthy, young subjects, doses of 200 IU and 4000 IU cholecalciferol were compared to placebo over a period of 28 days during winter. The overall mean baseline 25(OH)D level in this group was 32.2 ng/mL. No significant changes in 25(OH)D levels were observed in the placebo and 200 IU cholecalcifrol groups. However, significant elevations in 25(OH)D levels were apparent on weekly assessments in the 4000 IU cholecalciferol group with a mean elevation of approximately 17 ng/mL at the end of the study, compared to baseline. The effectiveness of a daily 4000 IU cholecalciferol dose was also reported in 2 earlier clinical trials. In a conceptually similar study, 30 slightly older, healthy patients with 25(OH)D levels ≤20 ng/mL, were randomized to receive either 2000 or 5000 IU cholecalciferol over a 3 month period. The 2000 IU group, which had a mean baseline 25(OH)D level of 16.5 ng/mL, experienced a mean increase of 14 ng/mL. The 5000 IU group, which had a mean baseline 25(OH)D level of 14.3 ng/mL, experienced a mean increase of 32 ng/mL. 45% vs. 93% of subjects achieved 25(OH)D levels >30 ng/mL in the 2000 IU vs. 5000 IU cholecalciferol groups. In a study involving 67 healthy males, daily cholecalciferol doses of 1000 IU, 5000 IU, and 10,000 IU were compared to placebo over a period of 20 weeks. Daily 1000 IU cholecalciferol was associated with a mean elevation in 25(OH)D levels of 4.8 ng/mL at steady state, which was achieved at approximately 30 days; a daily dose of 5000 IU cholecalciferol was associated with a mean elevation in 25(OH)D levels of 36.6 ng/mL at steady state, which was achieved at approximately 100 days; and finally, a daily dose of 10,000 IU cholecalciferol was associated with a mean elevation in 25(OH)D levels of 63.5 ng/mL at steady state, which was achieved at approximately 120 days. Though study compliance was acceptable in all of studies, adherence to a daily schedule may not be a realistic expectation in the general population.
Based on such concerns, there is a growing trend in the literature to evaluate the effect of mega-bolus doses of vitamin D supplements on 25(OH)D levels. The effect of a single 100,000 IU cholecalciferol dose in 30 healthy subjects with a mean baseline 25(OH)D level of 24 ng/mL was shown to produce a mean peak rise of 15 ng/mL at about 7 days post-supplementation. 25(OH)D levels dropped to <32 ng/mL by day 84 post-supplementation. The tolerability of such a dose was demonstrated in an earlier study, where 2686 elderly participants took either 100,000 IU cholecalciferol or placebo every 4 months for a duration of 5 years. In a more detailed study design, involving 224 women diagnosed with breast cancer, 3 different supplementation regimens based on pre-study 25(OH)D levels were compared over a period of 8-16 weeks. Women with 25(OH)D ≥32 ng/mL were prescribed no supplementation, while those with 25(OH)D 25 to <32 ng/mL were prescribed daily 1000 IU cholecalciferol (low dose supplementation group). The high dose supplementation group included women with 25(OH)D 15 to <25 ng/mL, who were prescribed weekly 50,000 IU cholecalciferol and women with 25(OH)D <15 ng/mL, who were prescribed weekly 100,000 IU cholecalciferol. Mean change in 25(OH)D levels were 3.1 ng/mL, 9.4 ng/mL, and 24.3 ng/mL in the no supplementation, low dose supplementation, and high dose supplementation groups, respectively. With continued concerns over patient compliance and the need for frequent checks, an annual dose of 500,000 IU cholecalciferol was administered to 102 elderly, community-dwelling females for 3-5 years. Mean 25(OH)D levels was 28 ng/mL immediately before the second dose. Mean 1-month and median 3-month post supplementation 25(OH)D levels were 49 ng/mL and 36 ng/mL, respectively. Similarly, 12 home-dwelling, elderly subjects were given a single oral dose of 600,000 IU cholecalciferol. Mean baseline 25(OH)D was 21.7 ng/mL with a mean peak increment to 67.1 ng/mL (Δ 45.4 ng/mL) on day 3 post-supplementation. Mean 25(OH)D levels were down to 35.2 ng/mL by day 90 post-supplementation.
It is important to note that none of the patients in the daily regimen or bolus dose studies discussed above experienced vitamin D toxicity, despite many patients achieving 25(OH)D levels above the IOM’s “safe” threshold of 50 ng/mL. In fact, the majority of published reports suggest that even early signs and symptoms of vitamin D toxicity (hypercalcuria and hypercalcemia) do not appear until 25(OH)D levels exceed 200 ng/mL. Application of a conservative “uncertainty factor” of 2 would indicate that an upper threshold for 25(OH)D levels may be 100 ng/mL. The maximum daily dose of cholecalciferol is also debatable, since reports of vitamin D toxicity have only been reported with doses >40,000 IU per day. The reported maximum tolerable dose of cholecalciferol, used over an extended period of time, is nonetheless 50,000 IU. Application of a conservative “safety factor” of 5 would indicate that an upper threshold for daily cholecalciferol dosing may be 10,000 IU. Certainly, the extended use of such a dose has been demonstrated to be safe and is estimated to be equivalent to the natural production of 25(OH)D upon liberal skin exposure to sunlight.
CONCLUSION
Association studies point to a clinically significant relationship between 25(OH)D levels and the risk of all-cause mortality, cardiovascular disease, pulmonary ailments, diabetes mellitus, and cancer. Yet, RCTs to date, limited by small sample sizes, heterogeneous dosing schedules, and varying study end-points, have been less persuasive. High quality RCTs are needed to determine: 1) optimal 25(OH)D levels for overall health; 2) whether vitamin D supplementation can improve outcomes; and 3) how to dose supplements in order to achieve optimal 25(OH)D levels.
Based on existing evidence, a target 25(OH)D range of 30-50 ng/mL would most likely optimize potential health-related benefits of vitamin D and minimize the potential for harm. Although a maximum safe level for 25(OH)D may be 100 ng/mL, additional health benefits with levels between 50-100 ng/mL are not apparent. As such, depending on baseline levels, daily cholecalciferol dosing of either 5000 IU or 10,000 IU appears to be safe and effective in restoring 25(OH)D levels to a therapeutic range. Bolus doses between 50,000 and 600,000 IU have been studied in the general population and are thought to be safe (although studies with doses >150,000 IU have generally involved a small number of subjects). The selection of a bolus regimen should take into consideration the desired elevation in 25(OH)D and frequency of dosing. Since 25(OH)D levels peak between days 3 and 7 following a bolus (depending on the size of the bolus dose), this provide a “monitoring window” to assess either adequacy of supplementation or potential for toxicity. There is currently insufficient evidence to provide guidance regarding a combined bolus and daily supplementation regimen. However, this may provide a reasonable approach when the goal is to rapidly restore and then maintain 25(OH)D levels in severely deficient patients. Any intensive vitamin D repletion program should, of course, be considered in the context of individual patient co-morbidities and desired outcomes.
FUNDING
Dr. Quraishi received support from the National Institutes of Health grants 5T32GM007592-33 (Harvard Anaesthesia Center) and UL1 RR025758 (Harvard Scholars in Clinical Science Program).
Dr. Camargo Jr received support from the National Institutes of Health grants R01 AI093723 and U01 AI087881.
DISCLOSURE OF INTERESTS
Dr. Quraishi serves on the Board of Directors of the Vitamin D Council.
REFERENCES
- Adams JS, Hewison M. Update in vitamin D.
- Ginde AA, Liu MC, Camargo CA Jr. Demographic differences and trends of vitamin D insufficiency in the US population, 1988-2004.
- Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, et al. The 2011 report on dietary reference intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know.
- Heaney RP, Holick MF. Why the IOM recommendations for vitamin D are deficient.
- Moreno LA, Valtueña J, Pérez-López F, González-Gross M. Health effects related to low vitamin d concentrations: beyond bone metabolism.
- Kulie T, Groff A, Redmer J, Hounshell J, Schrager S. Vitamin D: an evidence-based review.
- Vacek JL, Vanga SR, Good M, Lai SM, Lakkireddy D, Howard PA. Vitamin d deficiency and supplementation and relation to cardiovascular health.
- Lappe JM, Travers-Gustafson D, Davies KM, Recker RR, Heaney RP. Vitamin D and calcium supplementation reduces cancer risk: results of a randomized trial.
- Laaksi I, Ruohola JP, Mattila V, Auvinen A, Ylikomi T, Pihlajamäki H. Vitamin D supplementation for the prevention of acute respiratory tract infection: a randomized, double-blinded trial among young Finnish men.
- Autier P, Gandini S. Vitamin D supplementation and total mortality: a meta-analysis of randomized controlled trials.
- Bjelakovic G, Gluud LL, Nikolova D, Whitfield K, Wetterslev J, Simonetti RG, et al. Vitamin D supplementation for prevention of mortality in adults.
- de Paula FJA, Rosen CJ. Vitamin D safety and requirements.
- Lai JKC, Lucas RM, Clements MS, Harrison SL, Banks E. Assessing vitamin D status: pitfalls for the unwary.
- Heaney RP, Recker RR, Grote J, Horst RL, Armas LAG. Vitamin D(3) is more potent than vitamin D(2) in humans.
- Glendenning P, Inderjeeth CA. Screening for vitamin D deficiency: defining vitamin D deficiency, target thresholds of treatment and estimating the benefits of treatment.
- Henry HL. Regulation of vitamin D metabolism. Best Pract.
- Amrein K, Venkatesh B. Vitamin D and the critically ill patient.
- Zittermann A. Vitamin D in preventive medicine: are we ignoring the evidence?
- Passeri G, Pini G, Troiano L, Vescovini R, Sansoni P, Passeri M, et al. Low vitamin D status, high bone turnover, and bone fractures in centenarians.
- Cashman KD, Kiely M. Towards prevention of vitamin D deficiency and beyond: knowledge gaps and research needs in vitamin D nutrition and public health.
- Biesalski HK. Vitamin D recommendations: beyond deficiency.
- Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline.
- Durazo-Arvizu RA, Dawson-Hughes B, Sempos CT, Yetley EA, Looker AC, Cao G, et al. Three-phase model harmonizes estimates of the maximal suppression of parathyroid hormone by 25-hydroxyvitamin D in persons 65 years of age and older.
- Holick MF. Vitamin D: A millenium perspective.
- White JH. Vitamin D metabolism and signaling in the immune system.
- Schwalfenberg GK. A review of the critical role of vitamin D in the functioning of the immune system and the clinical implications of vitamin D deficiency.
- Aranow C. Vitamin D and the immune system.
- Sigmundsdottir H. From the bench to the clinic: New aspects on immunoregulation by vitamin D analogs.
- Clendenen TV, Koenig KL, Arslan AA, Lukanova A, Berrino F, Gu Y, et al. Factors associated with inflammation markers, a cross-sectional analysis.
- White JH. Regulation of intracrine production of 1,25-dihydroxyvitamin D and its role in innate immune defense against infection.
- Wu S, Sun J. Vitamin D, vitamin D receptor, and macroautophagy in inflammation and infection.
- Méndez-Samperio P. The human cathelicidin hCAP18/LL-37: a multifunctional peptide involved in mycobacterial infections.
- Bhan I, Camargo CA Jr, Wenger J, Ricciardi C, Ye J, Borregaard N, et al. Circulating levels of 25-hydroxyvitamin D and human cathelicidin in healthy adults.
- Dobnig H, Pilz S, Scharnagl H, Renner W, Seelhorst U, Wellnitz B, et al. Independent association of low serum 25-hydroxyvitamin d and 1,25-dihydroxyvitamin d levels with all-cause and cardiovascular mortality.
- Melamed ML, Michos ED, Post W, Astor B. 25-hydroxyvitamin D levels and the risk of mortality in the general population.
- Ginde AA, Scragg R, Schwartz RS, Camargo CA Jr. Prospective study of serum 25-hydroxyvitamin D level, cardiovascular disease mortality, and all-cause mortality in older US. adults.
- Grant WB. An estimate of the global reduction in mortality rates through doubling vitamin D levels.
- Akin F, Ayça B, Köse N, Duran M, Sar M, Uysal OK, et al. Serum Vitamin D Levels Are Independently Associated With Severity of Coronary Artery Disease.
- Wang TJ, Pencina MJ, Booth SL, Jacques PF, Ingelsson E, Lanier K, et al. Vitamin D deficiency and risk of cardiovascular disease.
- Khalili H, Talasaz AH, Salarifar M. Serum vitamin D concentration status and its correlation with early biomarkers of remodeling following acute myocardial infarction.
- Kestenbaum B, Katz R, de Boer I, Hoofnagle A, Sarnak MJ, Shlipak MG, et al. Vitamin D, parathyroid hormone, and cardiovascular events among older adults.
- Sugden JA, Davies JI, Witham MD, Morris AD, Struthers AD. Vitamin D improves endothelial function in patients with Type 2 diabetes mellitus and low vitamin D levels.
- Salehpour A, Shidfar F, Hosseinpanah F, Vafa M, Razaghi M, Hoshiarrad A, et al. Vitamin D3 and the risk of CVD in overweight and obese women: a randomised controlled trial.
- Vaidya A, Sun B, Forman JP, Hopkins PN, Brown NJ, Kolatkar NS, et al. The Fok1 vitamin D receptor gene polymorphism is associated with plasma renin activity in Caucasians.
- Shirts BH, Howard MT, Hasstedt SJ, Nanjee MN, Knight S, Carlquist JF, et al. Vitamin D dependent effects of APOA5 polymorphisms on HDL cholesterol.
- Ortlepp JR, Korff von A, Hanrath P, Zerres K, Hoffmann R. Vitamin D receptor gene polymorphism BsmI is not associated with the prevalence and severity of CAD in a large-scale angiographic cohort of 3441 patients.
- Nnoaham KE, Clarke A. Low serum vitamin D levels and tuberculosis: a systematic review and meta-analysis.
- Martineau AR, Wilkinson RJ, Wilkinson KA, Newton SM, Kampmann B, Hall BM, et al. A single dose of vitamin D enhances immunity to mycobacteria.
- Nursyam EW, Amin Z, Rumende CM. The effect of vitamin D as supplementary treatment in patients with moderately advanced pulmonary tuberculous lesion.
- Martineau AR, Timms PM, Bothamley GH, Hanifa Y, Islam K, Claxton AP, et al. High-dose vitamin D3 during intensive-phase antimicrobial treatment of pulmonary tuberculosis: a double-blind randomised controlled trial.
- Sutherland ER, Goleva E, Jackson LP, Stevens AD, Leung DYM. Vitamin D levels, lung function, and steroid response in adult asthma.
- Devereux G, Wilson A, Avenell A, McNeill G, Fraser WD. A case-control study of vitamin D status and asthma in adults.
- Hughes AM, Lucas RM, Ponsonby AL, Chapman C, Coulthard A, Dear K, et al. The role of latitude, ultraviolet radiation exposure and vitamin D in childhood asthma and hayfever: an Australian multicenter study.
- Searing DA, Zhang Y, Murphy JR, Hauk PJ, Goleva E, Leung DYM. Decreased serum vitamin D levels in children with asthma are associated with increased corticosteroid use.
- Goleva E, Searing DA, Jackson LP, Richers BN, Leung DYM. Steroid requirements and immune associations with vitamin D are stronger in children than adults with asthma.
- Poon AH, Laprise C, Lemire M, Montpetit A, Sinnett D, Schurr E, et al. Association of vitamin D receptor genetic variants with susceptibility to asthma and atopy.
- Raby BA, Lazarus R, Silverman EK, Lake S, Lange C, Wjst M, et al. Association of vitamin D receptor gene polymorphisms with childhood and adult asthma.
- Cannell JJ, Vieth R, Umhau JC, Holick MF, Grant WB, Madronich S, et al. Epidemic influenza and vitamin D.
- White ANJ, Ng V, Spain CV, Johnson CC, Kinlin LM, Fisman DN. Let the sun shine in: effects of ultraviolet radiation on invasive pneumococcal disease risk in Philadelphia, Pennsylvania.
- Leow L, Simpson T, Cursons R, Karalus N, Hancox RJ. Vitamin D, innate immunity and outcomes in community acquired pneumonia.
- Sabetta JR, DePetrillo P, Cipriani RJ, Smardin J, Burns LA, Landry ML. Serum 25-hydroxyvitamin d and the incidence of acute viral respiratory tract infections in healthy adults.
- Laaksi I, Ruohola JP, Tuohimaa P, Auvinen A, Haataja R, Pihlajamäki H, et al. An association of serum vitamin D concentrations.
- Ginde AA, Mansbach JM, Camargo CA Jr. Association between serum 25-hydroxyvitamin D level and upper respiratory tract infection in the Third National Health and Nutrition Examination Survey.
- Berry DJ, Hesketh K, Power C, Hyppönen E. Vitamin D status has a linear association with seasonal infections and lung function in British adults.
- Aloia JF, LI-NG M. Re: epidemic influenza and vitamin D.
- Wolfenden LL, Judd SE, Shah R, Sanyal R, Ziegler TR, Tangpricha V. Vitamin D and bone health in adults with cystic fibrosis.
- Stephenson A, Brotherwood M, Robert R, Atenafu E, Corey M, Tullis E. Cholecalciferol significantly increases 25-hydroxyvitamin D concentrations in adults with cystic fibrosis.
- Pincikova T, Nilsson K, Moen IE, Karpati F, Fluge G, Hollsing A, et al. Inverse relation between vitamin D and serum total immunoglobulin G in the Scandinavian Cystic Fibrosis Nutritional Study.
- Black PN, Scragg R. Relationship between serum 25-hydroxyvitamin d and pulmonary function in the third national health and nutrition examination survey.
- Ferrari M, Schenk K, Papadopoulou C, Ferrari P, Dalle Carbonare L, Bertoldo F. Serum 25-hydroxy vitamin D and exercise capacity in COPD.
- Janssens W, Bouillon R, Claes B, Carremans C, Lehouck A, Buysschaert I, et al. Vitamin D deficiency is highly prevalent in COPD and correlates with variants in the vitamin D-binding gene.
- Lehouck A, Mathieu C, Carremans C, Baeke F, Verhaegen J, Van Eldere J, et al. High doses of vitamin D to reduce exacerbations in chronic obstructive pulmonary disease: a randomized trial.
- Hyppönen E, Läärä E, Reunanen A, Järvelin MR, Virtanen SM. Intake of vitamin D and risk of type 1 diabetes: a birth-cohort study.
- Zipitis CS, Akobeng AK. Vitamin D supplementation in early childhood and risk of type 1 diabetes: a systematic review and meta-analysis.
- Mohr SB, Garland FC, Garland CF, Gorham ED, Ricordi C. Is there a role of vitamin D deficiency in type 1 diabetes of children?
- Zhang J, Li W, Liu J, Wu W, Ouyang H, Zhang Q, et al. Polymorphisms in the vitamin D receptor gene and type 1 diabetes mellitus risk: an update by meta-analysis.
- Chiu KC, Chu A, Go VLW, Saad MF. Hypovitaminosis D is associated with insulin resistance and ß cell dysfunction.
- Karnchanasorn R, Ou H. Plasma 25-Hydroxyvitamin D Levels Are Favorably Associated With [beta]-Cell Function.
- Pittas AG, Harris SS, Stark PC, Dawson-Hughes B. The effects of calcium and vitamin D supplementation on blood glucose and markers of inflammation in nondiabetic adults.
- Forouhi NG, Ye Z, Rickard AP, Khaw KT, Luben R, Langenberg C, et al. Circulating 25-hydroxyvitamin D concentration and the risk of type 2 diabetes: results from the European Prospective Investigation into Cancer (EPIC)-Norfolk cohort and updated meta-analysis of prospective studies.
- González-Molero I, Rojo-Martínez G, Morcillo S, Gutiérrez-Repiso C, Rubio-Martín E, Almaraz MC, et al. Vitamin D and incidence of diabetes: A prospective cohort study.
- Bid HK, Konwar R, Aggarwal CG, Gautam S, Saxena M, Nayak VL, et al. Vitamin D receptor (FokI, BsmI and TaqI) gene polymorphisms and type 2 diabetes mellitus: a North Indian study.
- Dilmec F, Uzer E, Akkafa F, Kose E, van Kuilenburg ABP. Detection of VDR gene ApaI and TaqI polymorphisms in patients with type 2 diabetes mellitus using PCR-RFLP method in a Turkish population.
- Malecki M, Klupa T, Wolkow P, Bochenski J, Wanic K, Sieradzki J. Association study of the vitamin D: 1alpha-hydroxylase (CYP1alpha) gene and type 2 diabetes mellitus in a Polish population.
- Malecki M, Frey J, Moczulski D, Klupa T, Kozek E, Sieradzki J. Vitamin D receptor gene polymorphisms and association with type 2 diabetes mellitus in a Polish population.
- Valdivielso JM, Fernandez E. Vitamin D receptor polymorphisms and diseases.
- Avenell A, Maclennan GS, Jenkinson DJ, McPherson GC, McDonald AM, Pant PR, et al. Long-Term Follow-Up for Mortality and Cancer in a Randomized Placebo-Controlled Trial of Vitamin D3 and/or Calcium (RECORD Trial).
- Giovannucci E, Liu Y, Rimm EB, Hollis BW, Fuchs CS, Stampfer MJ, et al. Prospective study of predictors of vitamin D status and cancer incidence and mortality in men.
- Freedman DM, Looker AC, Chang SC, Graubard BI. Prospective study of serum vitamin D and cancer mortality in the United States.
- Lee JE. Circulating levels of vitamin D, vitamin D receptor polymorphisms, and colorectal adenoma: a meta-analysis.
- Gorham ED, Garland CF, Garland FC, Grant WB, Mohr SB, Lipkin M, et al. Optimal vitamin D status for colorectal cancer prevention: a quantitative meta analysis.
- Touvier M, Chan DSM, Lau R, Aune D, Vieira R, Greenwood DC, et al. Meta-analyses of vitamin D intake, 25-hydroxyvitamin D status, vitamin D receptor polymorphisms, and colorectal cancer risk.
- Lin J, Manson JE, Lee IM, Cook NR, Buring JE, Zhang SM. Intakes of calcium and vitamin D and breast cancer risk in women.
- Yin L, Grandi N, Raum E, Haug U, Arndt V, Brenner H. Meta-analysis: serum vitamin D and breast cancer risk.
- Gandini S, Boniol M, Haukka J, Byrnes G, Cox B, Sneyd MJ, et al. Meta-analysis of observational studies of serum 25-hydroxyvitamin D levels and colorectal, breast and prostate cancer and colorectal adenoma.
- Köstner K, Denzer N, Müller CSL, Klein R, Tilgen W, Reichrath J. The relevance of vitamin D receptor (VDR) gene polymorphisms for cancer: a review of the literature.
- Dorjgochoo T, Delahanty R, Lu W, Long J, Cai Q, Zheng Y, et al. Common genetic variants in the vitamin D pathway including genome-wide associated variants are not associated with breast cancer risk among Chinese women.
- McKay JD, McCullough ML, Ziegler RG, Kraft P, Saltzman BS, Riboli E, et al. Vitamin D receptor polymorphisms and breast cancer risk: results from the National Cancer Institute Breast and Prostate Cancer Cohort Consortium.
- Tang C, Chen N, Wu M, Yuan H, Du Y. Fok1 polymorphism of vitamin D receptor gene contributes to breast cancer susceptibility: a meta-analysis.
- Anderson LN, Cotterchio M, Cole DEC, Knight JA. Vitamin D-related genetic variants, interactions with vitamin D exposure, and breast cancer risk among Caucasian women in Ontario.
- Yin L, Raum E, Haug U, Arndt V, Brenner H. Meta-analysis of longitudinal studies: Serum vitamin D and prostate cancer risk.
- Gilbert R, Martin RM, Beynon R, Harris R, Savovic J, Zuccolo L, et al. Associations of circulating and dietary vitamin D with prostate cancer risk: a systematic review and dose-response meta-analysis.
- Travis RC, Crowe FL, Allen NE, Appleby PN, Roddam AW, Tjønneland A, et al. Serum vitamin D and risk of prostate cancer in a case-control analysis nested within the European Prospective Investigation into Cancer and Nutrition (EPIC).
- Luxwolda MF, Kuipers RS, Kema IP, Janneke Dijck-Brouwer DA, Muskiet FAJ. Traditionally living populations in East Africa have a mean serum 25-hydroxyvitamin D concentration of 115 nmol/l.
- Barker T, Martins TB, Hill HR, Kjeldsberg CR, Henriksen VT, Dixon BM, et al. Different doses of supplemental vitamin D maintain interleukin-5 without altering skeletal muscle strength: a randomized, double-blind, placebo-controlled study in vitamin D sufficient adults.
- Vieth R, Chan PC, MacFarlane GD. Efficacy and safety of vitamin D3 intake exceeding the lowest observed adverse effect level.
- Vieth R, Kimball S, Hu A, Walfish PG. Randomized comparison of the effects of the vitamin D3 adequate intake versus 100 mcg (4000 IU) per day on biochemical responses and the wellbeing of patients.
- Diamond T, Wong YK, Golombick T. Effect of oral cholecalciferol 2,000 versus 5,000 IU on serum vitamin D, PTH, bone and muscle strength in patients with vitamin D deficiency.
- Heaney RP, Davies KM, Chen TC, Holick MF, Barger-Lux MJ. Human serum 25-hydroxycholecalciferol response to extended oral dosing with cholecalciferol.
- Ilahi M, Armas LAG, Heaney RP. Pharmacokinetics of a single, large dose of cholecalciferol.
- Trivedi DP, Doll R, Khaw KT. Effect of four monthly oral vitamin D3 (cholecalciferol) supplementation on fractures and mortality in men and women living in the community: randomised double blind controlled trial.
- Peppone LJ, Huston AJ, Reid ME, Rosier RN, Zakharia Y, Trump DL, et al. The effect of various vitamin D supplementation regimens in breast cancer patients.
- Sanders KM, Stuart AL, Williamson EJ, Jacka FN, Dodd S, Nicholson G, et al. Annual high-dose vitamin D3 and mental well-being: randomised controlled trial.
- Rossini M, Gatti D, Viapiana O, Fracassi E, Idolazzi L, Zanoni S, et al. Short-Term Effects on Bone Turnover Markers of a Single High Dose of Oral Vitamin D3.
- Vieth R. Critique of the considerations for establishing the tolerable upper intake level for vitamin D: critical need for revision upwards.
- Vieth R. Vitamin D toxicity, policy, and science.
- Jones G. Pharmacokinetics of vitamin D toxicity.
- Heaney RP. Vitamin D: criteria for safety and efficacy.
- Glade MJ. A 21st century evaluation of the safety of oral vitamin D.
- Vieth R. Vitamin D supplementation, 25-hydroxyvitamin D concentrations, and safety.
- Barger-Lux MJ, Heaney RP, Dowell S, Chen TC, Holick MF. Vitamin D and its major metabolites: serum levels after graded oral dosing in healthy men.
- Hathcock JN, Shao A, Vieth R, Heaney R. Risk assessment for vitamin D.
- Holick MF. Sunlight “D”ilemma: risk of skin cancer or bone disease and muscle weakness.